Students get through the TN Board 11th Bio Zoology Important Questions Chapter 8 Excretion which is useful for their exam preparation.
TN State Board 11th Bio Zoology Important Questions Chapter 8 Excretion
Answer the following.
Question 1.
Mention the three homeostatic processes of kidneys.
Answer:
Three homeostatic processes namely, osmotic regulation, ionic regulation, and nitrogen excretion.
Question 2.
Define the following terms, (i) Osmotic regulation, (ii) Ionic regulation, (iii) Nitrogen excretion.
Answer:
- Osmotic regulation is the control of tissue osmotic pressure which acts as a driving force for the movement of water across biological membranes.
- Ionic regulation is the control of the ionic composition of body fluids.
- The process by which the body gets rid of the nitrogenous waste products of protein metabolism is called excretion. Nitrogen excretion is the pathway by which animals excrete ammonia, the toxic nitrogenous end product of protein catabolism.
Question 3.
Differentiate osmoconformers from osmoregulators.
Answer:
| Osmoconformers | Osmoregulators |
| Osmoconformers are able to change their internal osmotic concentration with changes in the external environment, eg: marine molluscs and sharks. | Osmoregulators maintain their internal osmotic concentration irrespective of their external osmotic environment, eg: Otters. |
![]()
Question 4.
What are stenohaline and euryhaline animals?
Answer:
The stenohaline animals can tolerate only narrow fluctuations in the salt concentration (example Goldfish), whereas the euryhaline animals are able to tolerate wide fluctuations in the salt concentrations, eg: Artemia, tilapia, and salmons.
Question 5.
Define excretion.
Answer:
The process by which the body gets rid of the nitrogenous waste products of protein metabolism is called excretion.
Question 6.
What are the different waste products of protein metabolism?
Answer:
Waste products of protein metabolism are trimethylamine oxide (TMO) in marine teleosts, guanine in spiders, hippuric acid, allantoin, allantoic acid, ornithuric acid, creatinine, creatine, purines, pyrimidines, and pterines.
Question 7.
Name the three major nitrogenous waste materials.
Answer:
The major nitrogenous waste products are ammonia, urea, and uric acid.
Question 8.
What are ammonoteles, uricoteles and ureoteles.
Answer:
- Animals that excrete most of its nitrogen in the form of ammonia are called ammonoteles. Many fishes, aquatic amphibians and aquatic insects are ammOnotelic.
- Reptiles, birds, land snails and insects excrete uric acid crystals, with a minimum loss of water and are called uricoteles. In terrestrial animals, less toxic urea and uric acid are produced to conserve water.
- Mammals and terrestrial amphibians mainly excrete urea and are called ureoteles.
![]()
Question 9.
The animal kingdom shows a wide variety of excretory structures. Name some of the excretory organs and in which animals they are present as well as its functional aspect.
Answer:
- Protonephridia are excretory structures with specialized cells in the form of flame cells (cilia) in Platyhelminthes (tapeworm) and solenocytes (flagella) in Amphioxus.
- Nematodes have rennette cells, Metanephridia are the tubular excretory structures in annelids and molluscs.
- Malpighian tubules are the excretory structures in most insects.
- Antennal glands or green glands perform an excretory function in crustaceans like prawns.
Question 10.
What are the structures involved in the excretory system of humans? Write the structure of the kidney with a neat diagram.
Answer:
The excretory system in humans consists of a pair of kidneys, a pair of meters, urinary bladder, and urethra. Kidneys are reddish-brown, bean-shaped structures that lie in the superior lumbar region between the levels of the last thoracic and third lumber vertebra close to the dorsal inner wall of the abdominal cavity. The right kidney is placed slightly lower than the left kidney. Each kidney weighs an average of 120-170 grams. The outer layer of the kidney is covered by three layers of supportive tissues namely, renal fascia, perirenal fat capsule, and fibrous capsule.
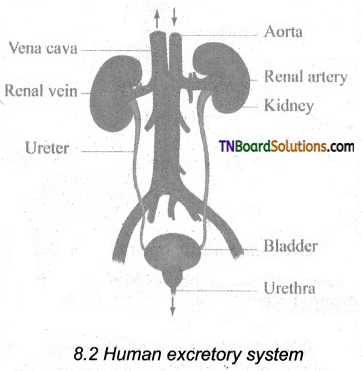
Question 11.
Describe the internal anatomy of the kidney with a neat diagram of L.S. of the kidney.
Answer:
The longitudinal section of the kidney shows an outer cortex, inner medulla, and pelvis. The medulla is divided into a few conical tissue masses called medullary pyramids or renal – pyramids. The part of the cortex that extends in between the medullary pyramids in the renal columns of Bertini. The center of the inner concave surface of the kidney has a notch Called the renal hilum, through which the ureter, blood vessels, and nerves innervate. Inner to the hilum is a broad funnel-shaped space called the renal pelvis with a projection called calyces. The renal pelvis is continuous with the ureter once it leaves the hilum. The walls of the calyces, pelvis, and ureter have smooth muscles which contract rhythmically. The calyces collect the urine and empties it into the ureter, which is stored in the urinary bladder temporarily. The urinary bladder opens into the urethra through which urine is expelled out.
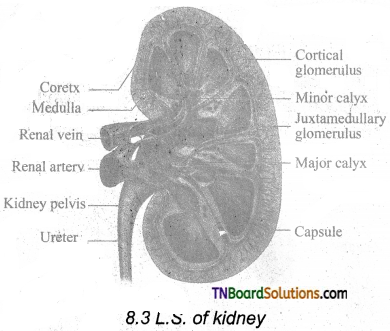
![]()
Question 12.
Give an account of the structure of the nephron with a suitable sketch.
Answer:
Each kidney has nearly one million complex tubular structures called nephrons. Each nephron consists of a filtering corpuscle called the renal corpuscle (malpighian body) and a renal tubule. The renal tubule opens into a longer tubule called the collecting duct.
The renal tubule begins with a double-walled cup-shaped structure called the Bowman’s capsule, which encloses a ball of capillaries that delivers fluid to the tubules, called the glomerulus. The bowman’s capsule and the glomerulus together constitute the renal corpuscle. The endothelium of the glomerulus has many pores (fenestrae). The external parietal layer of the Bowman’s capsule is made up of simple squamous epithelium and the visceral layer is made of epithelial cells called podocytes. The podocytes end in foot processes which cling to the basement membrane of the glomerulus. The openings between the foot processes are called filtration slits.
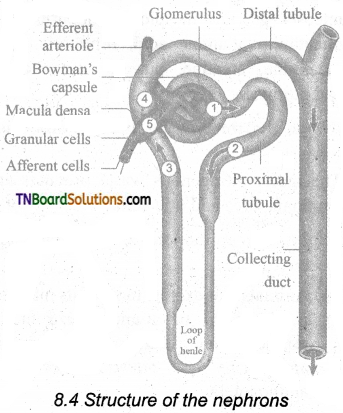
The renal tubule continues further to form the proximal convoluted tubule [PCT] followed by a U-shaped loop of Henle (Henle’s loop) that has a thin descending and a thick ascending limb. The ascending limb continues as a highly coiled tubular region called the distal convoluted tubule [DCT], The DCT of many nephrons opens into a straight tube called the collecting duct. The collecting duct runs through the medullary pyramids in the region of the pelvis. Several collecting ducts fuse to form a papillary duct that delivers urine into the calyces, which opens into the renal pelvis.
Question 13.
Write about the capillary bed of the nephrons.
Answer:
The capillary bed of the nephrons: First capillary bed of the nephron is the glomerulus and the other is the peritubular capillaries.
The glomerular capillary bed is different from other capillary beds in that it is supplied by the afferent and drained by the efferent arteriole. The efferent arteriole that comes out of the glomerulus forms a fine capillary network around the renal tubule called the peritubular capillaries. The efferent arteriole serving the juxtamedullary nephron forms bundles of a long straight vessel called vasa recta and runs parallel to the loop of Henle. Vasa recta are absent or reduced in cortical nephrons.
![]()
Question 14.
Name the steps involved in urine formation.
Answer:
Urine formation involves three main processes namely, glomerular filtration, tubular reabsorption, and tubular secretion.
Question 15.
Describe the process of glomerular filtration.
Answer:
Blood enters the kidney from the renal artery, into the glomerulus. Blood is composed of large quantities of water, colloidal proteins, sugars, salts, and nitrogenous end products. The first step in urine formation is the filtration of blood that takes place in the glomerulus. This is called glomerular filtration which is a passive process. The fluid that leaves the glomerular capillaries and enters the Bowman’s capsule is called the glomerular filtrate. The glomerular membrane has a large surface area and is more permeable to water and small molecules present in the blood plasma. Blood enters the glomerulus faster with greater force through the afferent arteriole and leaves the glomerulus through the efferent arterioles, much slower. This force is because of the difference in sizes between the afferent and efferent arteriole (afferent arteriole is wider than efferent arteriole) and glomerular hydrostatic pressure which is around 55mm Hg.
Kidneys produce about 180l glomerular filtrate in 24 hours. The molecules such as water, glucose, amino acids, and nitrogenous substances pass freely from the blood into the glomerulus. Molecules larger than 5nm are barred from entering the tubule. Glomerular pressure is the chief force that pushes water and solutes out of the blood and across the filtration membrane. The glomerular blood pressure (approximately 55 mmHg) is much higher than in other capillary beds. The two opposing forces are contributed by the plasma proteins in the capillaries. These include colloidal osmotic pressure (30 mmHg) and capsular hydrostatic pressure (15 mmHg) due to the fluids in the glomerular capsule. The net filtration pressure of 10 mmHg is responsible for renal filtration.

The effective glomerular pressure of 10 mmHg results in ultrafiltration. Glomerular filtration rate (GFR) is the volume of filtrate formed min-1 in all nephrons (glomerulus) of both kidneys. In adults, the GFR is approximately 120-125 mL/min.
Question 16.
The glomerulus of the nephron filtered the blood, and it is called glomerular filtrate. While it is passed through the different segments of the nephron, certain substances are selectively reabsorbed. What is the substance reabsorbed and in which segment? Explain.
Answer:
- Tubular reabsorption: This involves the movement of the filtrate back into the circulation. The volume of filtrate formed per day is around 170-180 L and the urine released is around 1.5 L per day, i.e„ nearly 99% of the glomerular filtrate that has to be reabsorbed by the renal tubules as it contains certain substances needed by the body. This process is called selective reabsorption. Reabsorption takes place by the tubular epithelial cells in different segments of the nephron either by active transport or passive transport, diffusion, and osmosis.
- Proximal convoluted Tubule (PCT): Glucose, lactate, amino acids, Na+, and water in the filtrate are reabsorbed in the PCT. Sodium is reabsorbed by active transport through the sodium-potassium (Na+ – K+) pump in the PCT. Small amounts of urea and uric acid are also reabsorbed.
- Descending limb of Henle’s loop: It is permeable to water due to the presence of aquaporins, but not permeable to salts. Water is lost in the descending limb, hence Na+ and Cl– get concentrated in the filtrate.
- Ascending limb of Henle’s loop: It is impermeable to water but permeable to solutes such as Na+, Cl– and K+.
- The distal convoluted tubule: It recovers water and secretes potassium into the tubule. Na+, Cl– and water remain in the filtrate of the DCT. Most of the reabsorption from this point is dependent on the body’s needs and is regulated by hormones. Reabsorption of bicarbonate (HCO3–) takes place to regulate the blood pH. Homeostasis of K+ and Na+ in the blood is also regulated in this region.
- Collecting duct: It is permeable to water, secretes K+ (potassium ions are actively transported into the tubule), and reabsorbs Na+ to produce concentrated urine.
![]()
Question 17.
How ADH by means of a feedback system regulates the function of kidneys.
Answer:
The functioning of kidneys is efficiently monitored and regulated by hormonal feedback control mechanisms involving the hypothalamus, juxtaglomerular apparatus, and to a certain extent the heart. Osmoreceptors in the hypothalamus are activated by changes in blood volume, body fluid volume, and ionic concentration. When there is excessive loss of fluid from the body or when there is an increase in blood pressure, the osmoreceptors of the hypothalamus respond by stimulating the neurohypophysis to secrete the antidiuretic hormone (ADH) or vasopressin (positive feedback). ADH facilitates the reabsorption of water by increasing the number of aquaporins on the cell surface membrane of the distal convoluted tubule and collecting duct. This increase in aquaporins causes the movement of water from the lumen into the interstitial cells, thereby preventing excess loss of water by diuresis. When you drink excess amounts of your favorite juice, osmoreceptors of the hypothalamus are no longer stimulated and the release of ADH is suppressed from the neurohypophysis (negative feedback) and the aquaporins of the collecting ducts move into the cytoplasm. This makes the collecting ducts impermeable to water and the excess fluid flows down the collecting duct without any water loss. Hence dilute urine is produced to maintain the blood volume.
Question 18.
What is diabetes insipidus? How is it called? What are the symptoms?
Answer:
- Vasopressin secretion is controlled by positive and negative feedback mechanisms.
- Defects in ADH receptors or the inability to secrete ADH leads to a condition called diabetes insipidus.
- Characterized by excessive thirst and excretion of large quantities of dilute urine resulting in dehydration and fall in blood pressure.
Question 19.
What is the role of ANF in kidneys? How it acts antagonistically to the renin-angiotensin system?
Answer:
Atrial Natriuretic factor: Excessive stretch of cardiac atrial cells cause an increase in blood flow to the atria of the heart and release Atrial Natriuretic Peptide or factor (ANF) travels to the kidney where it increases Na+ excretion and increases the blood flow to the glomerulus, acting on the afferent glomerular arterioles as a vasodilator or on efferent arterioles as a vasoconstrictor. It decreases aldosterone release from the adrenal cortex and also decreases the release of renin, thereby decreasing angiotensin II. ANF acts antagonistically to the renin-angiotensin system, aldosterone, and vasopressin.
Question 20.
What are the clinical diagnostic results of testing urine in case of diabetes mellitus?
Answer:
The presence of glucose (glucosuria) and ketone bodies (ketonuria) in the urine are indications of diabetes mellitus.
![]()
Question 21.
In what situation there is a chance for the production of hypotonic urine.
Answer:
Hypotonic urine is formed when the osmotic pressure of the body fluid is decreased due to water retention or solute loss when ADH secretion is lowered. If you drink a large volume of water without eating anything salty, the total body fluid volume increases quickly and the osmolarity decreases. The kidneys increase the volume of urine excreted.
Question 22.
Name and the role played by the other organs in excretion apart from kidneys.
Answer:
- Apart from kidneys, organs such as lungs, liver, and skin help to remove wastes.
- Our lungs remove large quantities of carbon dioxide (181/day) and significant quantities of water every day.
- The liver secretes bile containing substances like, bilirubin and biliverdin, cholesterol, steroid hormones,, vitamins and drugs which are excreted out along with the digestive wastes.
- Sweat and sebaceous glands in the skin eliminate certain wastes through their secretions.
- The sweat produced by the sweat glands primarily helps to cool the body and secondarily excretes Na+ and Cl–, small quantities of urea and lactate. Sebaceous glands eliminate certain substances like sterols, hydrocarbons, and waxes through sebum that provides a protective oily covering for the skin.
- Small quantities of nitrogenous wastes are also excreted through saliva.
Question 23.
Write some disorders caused in relation to the excretory system in humans.
Answer:
Urinary tract infection: Female’s urethra is very short and its external opening is close to the anal opening, hence improper toilet habits can easily carry faecal bacteria into the urethra. The urethral mucosa is continuous with the urinary tract and the inflammation of the urethra (urethritis) can ascend the tract to cause bladder inflammation (cystitis) or even renal inflammation (pyelitis or pyelonephritis). Symptoms include dysuria (painful urination), urinary urgency, fever, and sometimes cloudy or blood-tinged urine. When the kidneys are inflamed, back pain and severe headache often occur. Most urinary tract infections can be treated by antibiotics.
Renal Failure (Kidney Failure): Failure of the kidneys to excrete wastes may lead to accumulation of urea with a marked reduction in the urine output. Renal failure is of two types, Acute, and chronic renal failure. In acute renal failure, the kidney stops its function abruptly, but there are chances for recovery of kidney functions. In chronic renal failure, there is a progressive loss of .function of the nephrons which gradually decreases the function of kidneys.
Uremia: Uremia is characterized by an increase in urea and other non-protein nitrogenous substances like uric acid and creatinine in the blood. The normal urea level in human blood is about 17-30mg/100mL of blood. The urea concentration rises to 10 times normal levels during chronic renal failure.
Renal calculi: Renal calculi, also called renal stone or nephrolithiasis, is the formation of hard stone-like masses in the renal tubules of the renal pelvis. It is mainly due to the accumulation of soluble crystals of salts of sodium oxalates and certain phosphates.
This results in severe pain called “renal colic pain” and can cause scars in the kidneys. Renal stones can be removed by techniques like pyleothotomy or lithotripsy.
Glomerulonephritis: It is also called Bright’s disease and is characterized by inflammation of the glomeruli of both kidneys and is usually due to post-streptococcal infection that occurs in children. Symptoms are haematuria, proteinuria, salt and water retention, oliguria, hypertension, and pulmonary oedema.
![]()
Question 24.
Why is females, urinary infection is more easy and common than in males?
Answer:
The Female’s urethra is very short and its external opening is close to the anal opening, hence improper toilet habits can easily carry faecal bacteria into the urethra. The urethral mucosa is continuous with the urinary tract and the inflammation of the urethra (urethritis) can ascend the tract to cause bladder inflammation (cystitis) or even renal inflammation.
Question 25.
Write about the hemodialysis process with schematic diagram, (or) Write about an artificial kidney used in the dialysis process.
Answer:
A dialyzing machine or an artificial kidney is connected to the patient’s body. A dialyzing machine consists of a long cellulose tube surrounded by the dialyzing fluid in a water bath. The patient’s blood is drawn from a convenient artery and pumped into the dialyzing unit after adding an anticoagulant like heparin. The tiny pores in the dialysis tube allow small molecules such as glucose, salts, and urea to enter the water bath, whereas blood cells and protein molecules do not enter these pores. This stage is similar to the filtration process in the glomerulus.
The dialyzing liquid in the water bath consists of a solution of salt and sugar in correct proportion in order to prevent the loss of glucose and essential salts from the blood. The cleared blood is then pumped back to the body through a vein.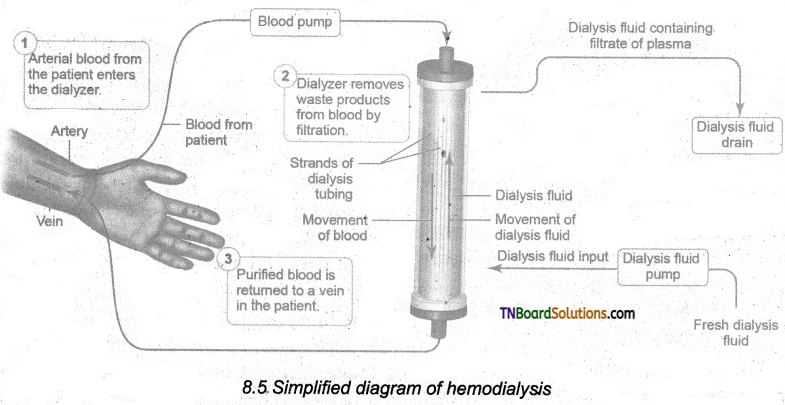
Question 26.
What is kidney transplantation? When and how it can be done?
Answer:
It is the ultimate method for the correction of acute renal failure. This involves the transfer of a healthy kidney from one person (donor) to another person with kidney failure. The donated kidney may be taken from a healthy person who is declared brain dead or from sibling or close relatives to minimize the chances of rejection by the immune system of the host. Immunosuppressive drugs are usually administered to the patient to avoid tissue rejection.
![]()
Question 27.
What are aquaporins?
Answer:
Aquaporins are Water-permeable channels (membrane transport proteins) that allow water to move across the epithelial cells in relation to the osmotic difference from the lumen to the interstitial fluid.
Question 28.
What is osmolarity? How is it expressed?
Answer:
Osmolarity – (The solute concentration of a solution of water is known as the osmolarity of the solution, expressed as milliosmoles /liter (mOsm/L).
Question 29.
Describe how the countercurrent multiplier mechanism helps in the formation of concentrated urine in humans.
Answer:
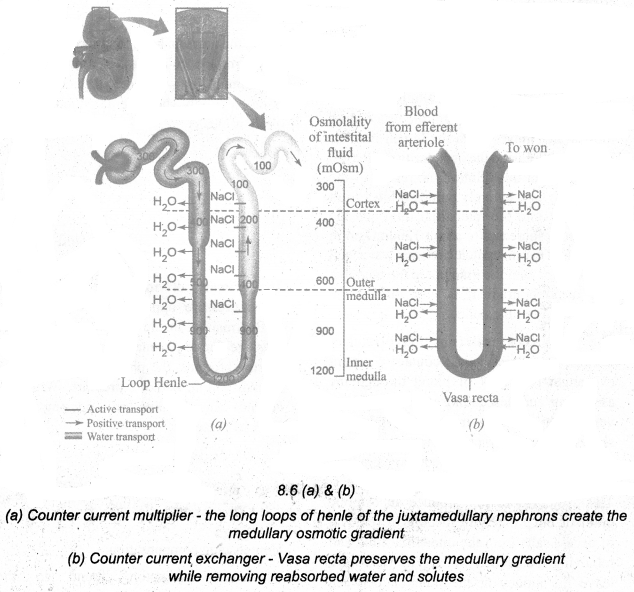
Formation of concentrated urine is accomplished by kidneys using counter current mechanisms. The major function of Henle’s loop is to concentrate Na+ and Cl–. There is low osmolarity near the cortex and high osmolarity towards the medulla. This osmolarity in the medulla is due to the presence of the solute transporters and is maintained by the arrangement of the loop of Henle, collecting duct, and vasa recta. This arrangement allows the movement of solutes from the filtrate to the interstitial fluid. At the transition between the proximal convoluted tubule and the descending loop of Henle, the osmolarity of the interstitial fluid is similar to that of the blood – about 300mOsm. Ascending and descending limbs of Henle, create a counter-current multiplier (interaction between flow of filtrate through the limbs of Henle’s and JMN) by active transport. Figure (a) shows, the countercurrent multiplier created by the long loops of Henle of the JM nephrons which creates a medullary osmotic gradient. As the fluid enters the descending limb, water moves from the lumen into the interstitial fluid, and the osmolarity decreases. To counteract this dilution the region of the ascending limb actively pumps solutes from the lumen into the interstitial fluid and the osmolarity increases to about 1200mOsm in the medulla. This mismatch between water and salts creates an osmotic gradient in the medulla. The osmotic gradient is also due to the permeability of the collecting duct to urea.
The vasa recta maintain the medullary osmotic gradient via countercurrent exchanger (the flow of blood through the ascending and descending vasa recta blood vessels) by passive transport. Figure (b) shows the counter current, exchanger where the vasa recta preserve the medullary gradient while removing reabsorbed Water and solutes. This system does not produce an osmotic gradient, but protects the medulla by removal of excess salts from the interstitial fluid and removing reabsorbed water. The vasa recta leaves the kidney at the junction between the cortex and medulla. The interstitial fluid at this point is iso-osmotic to the blood. When the blood leaves the efferent arteriole and enters the vasa recta the osmolarity in the medulla increases (1200mOsm) and results in passive uptake of solutes and loss of water. As the blood enters the cortex, the osmolarity in the blood decreases (300mOsm), and the blood loses solutes and gains water to form concentrated urine (hypertonic). Human kidneys can produce urine nearly four times concentrated than the initial filtrate formed.
![]()
Choose the correct answer.
1. Animals that can tolerate only narrow fluctuations in salt concentration are called:
(a) Osffioconformers
(b) Euryhaline
(c) Stenohaline
(d) Osmoregulators
Answer:
(c) Stenohaline
2. Which is euryhaline animal of the following?
(a) Tilapia
(b) gold fish
(c) sharks
(d) otters
Answer:
(a) Tilapia
3. The waste products of protein metabolism in spider is:
(a) Hippuric acid
(b) Quanine
(c) Allantonic
(d) Creatine
Answer:
(b) Quanine
4. Mammals and terrestrial amphibians mainly excrete urea and are called:
(a) Uricoteles
(b) Ammonoteles
(c) Ureoteles
(d) Gunotelic
Answer:
(c) Ureoteles
5. Each kidney of a human weighs about ………… gms.
(a) 120-280
(b) 120-270
(c) 130-170
(d) 120-170
Answer:
(d) 120-170
![]()
6. The primitive kidneys of invertebrates are called:
(a) protonephridia
(b) Mesonephridia
(c) Meganephridia
(d) malpighian tubules
Answer:
(a) protonephridia
7. (i) Flame cells (a) Nematodes
(ii) Solenocytes (b) Platyhelminthes
(iii) Renfiette cells (c) Amphioxus
(iv) Malpighian tubes (d) Insects
(a) (i)-(b), (ii)-(c), (iii)-(a), (iv)-(d)
(b) (i)-(c), (ii)-(b), (iii)-(d), (iv)-(a)
(c) (i)-(a), (ii)-(d), (iii)-(b), (iv)-(c)
(d) (a)-(d), (b)-(c), (c)-(a), (d)-(b)
Answer:
(b) (i)-(c), (ii)-(b), (iii)-(d), (iv)-(a)
8. The granular cells of the juxta glomerular apparatus secrete an enzyme called:
(a) thymin
(b) renin
(c) ADH
(d) angiotensin
Answer:
(d) angiotensin
9. The process of release of urine from the bladder is called:
(a) micturition
(b) malnutrition
(c) holozoic nutrition
(d) pasteurization
Answer:
(a) micturition
![]()
10. The formation of hard stone-like masses in the renal tubules is called:
(a) uremia
(b) gall stones
(c) bladder stone
(d) renal calculi
Answer:
(d) renal calculi
11. The renal stone is formed mainly by the accumulation of:
(a) salts of sodium oxalates and certain phosphates
(b) calcium and sodium
(c) creatinine
(d) potassium and phosphate
Answer:
(a) salts of sodium oxalates and certain phosphates
12. Renal stones can be removed by techniques like:
(a) dialysis
(b) medication
(c) lithotripsy
(d) holistic therapy
Answer:
(c) lithotripsy
13. Urine is a transparent yellowish fluid, because of the presence of the pigment called;
(a) chlorocruorirt
(b) cytochrome
(c) urochrome
(d) haemocyanin
Answer:
(c) urochrome
14. Animals that excrete of its nitrogen in the form of ammonia are called:
(a) ammonoteles
(b) uricoteles
(c) urioteles
(d) aminoteles
Answer:
(a) ammonoteles
![]()
15. Animals such as reptiles, birds and insects excrete,uric acid crystals with a minimum ross of water called:
(a) guanoteles
(b) uricoteles
(c) urioteles
(d) aminoteles
Answer:
(b) uricoteles
16. The excretory organ of platyhelminthes is:
(a) solenocytes
(b) flame cells
(c) rennette cells
(d) green glands
Answer:
(b) flame cells
17. ……… are the excretory structures in insects.
(a) Flame cells
(b) Antennal glands
(c) Malpighian tubules
(d) Solenocytes
Answer:
(c) Malpighian tubules
18. ………… is the structural and functional unit of kidneys.
(a) Neurons
(b) Malpighian tubules
(c) Nephrons
(d) Flame cells
Answer:
(c) Nephrons
19. Absense of ………… in Amphibians and freshwater fishes, produce dilute urine.
(a) Glomerulus
(b) Node of Ranvier
(c) Nephrons
(d) Henle’s loop
Answer:
(d) Henle’s loop
![]()
20. The ureter, blood vessels and nerves innervate the kidney through:
(a) ureter
(b) cortex
(c) medulla
(d) hilum
Answer:
(d) hilum
21. The biosynthesis of urea takes place in:
(a) blood
(b) kidney
(c) liver
(d) brain
Answer:
(c) liver
22. Defects of ADH receptors or inability to secrete ADH leads to a Condition called:
(a) diabetes mellitus
(b) diabetes insipidus
(c) Grave’s disease
(d) renal failure
Answer:
(b) diabetes insipidus
23. Increase in amount of urea in blood is called:
(a) nephritis
(b) Uremia
(c) Renal calculi
(d) cystitis
Answer:
(b) Uremia
![]()
24. ……….. is not a symptom of Renal failure.
(a) Increase in urea in blood
(b) Formation of hard stone like masses in renal tubules
(c) inflammation of the glomeruli
(d) all the above
Answer:
(d) all the above